This article needs more reliable medical references for verification or relies too heavily on primary sources. (October 2012) |  |
| Gynecologic ultrasonography | |
|---|---|
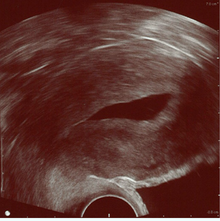
 Left hydrosalpinx on gynecologic ultrasonography | |
| Other names | Gynecologic sonography |
| ICD-9-CM | 88.76, 88.79 |
| OPS-301 code | 3-05d |
Gynecologic ultrasonography or gynecologic sonography refers to the application of medical ultrasonography to the female pelvic organs (specifically the uterus, the ovaries, and the fallopian tubes) as well as the bladder, the adnexa, and the recto-uterine pouch. The procedure may lead to other medically relevant findings in the pelvis.This technique is useful to detect myomas or mullerian malformations.
Routes


The examination can be performed by transabdominal ultrasonography, generally with a full bladder which acts as an acoustic window to achieve better visualization of pelvis organs, or by transvaginal ultrasonography with a specifically designed vaginal transducer. Transvaginal imaging utilizes a higher frequency imaging, which gives better resolution of the ovaries, uterus and endometrium (the fallopian tubes are generally not seen unless distended), but is limited to depth of image penetration, whereas larger lesions reaching into the abdomen are better seen transabdominally. Having a full bladder for the transabdominal portion of the exam is helpful because sound travels through fluid with less attenuation to better visualize the uterus and ovaries which lies posteriorly to the bladder. The procedure is by definition invasive when performed transvaginally. Scans are performed by health care professionals called sonographers, or gynecologists trained in ultrasound.
Applications
Gynecologic sonography is used extensively:
- to assess pelvic organs,
- to diagnose acute appendicitis[1]
- to diagnose and manage gynecologic problems including endometriosis, leiomyoma, adenomyosis, ovarian cysts and lesions,
- to identify adnexal masses, including ectopic pregnancy,
- to diagnose gynecologic cancer
- in infertility treatments to track the response of ovarian follicles to fertility medication (i.e. Pergonal). However, it often underestimates the true ovarian volume.[2]
Through transvaginal sonography ovarian cysts can be aspirated. This technique is also used in transvaginal oocyte retrieval to obtain human eggs (oocytes) through sonographic directed transvaginal puncture of ovarian follicles in IVF.
Gynecologic ultrasonography is sometimes overused when it is used to screen for ovarian cancer in women who are not at risk for this cancer.[3] There is consensus that women with only average risk for ovarian cancer should not be screened with this procedure for cancer.[3]
Sonohysterography
Sonohysterography is a specialized procedure by which fluid, usually sterile saline (then called saline infusion sonography or SIS), is instilled into the uterine cavity, and gynecologic sonography performed at the same time. A review in 2015 came to the conclusion that SIS is highly sensitive in the detection of intrauterine abnormalities in subfertile women, comparable to hysteroscopy. SIS is highly sensitive and specific test in the diagnosis of uterine polyps, submucous uterine fibroids, uterine anomalies and intrauterine adhesions (as part of Asherman's syndrome), and can be used as a screening tool for subfertile women prior to IVF treatment.[4]

See also
References
- ^ Caspi, B.; Zbar, AP.; Mavor, E.; Hagay, Z.; Appelman, Z. (Mar 2003). "The contribution of transvaginal ultrasound in the diagnosis of acute appendicitis: an observational study". Ultrasound Obstet Gynecol. 21 (3): 273–6. doi:10.1002/uog.72. PMID 12666223. S2CID 39843514.
- ^ Rosendahl M, Ernst E, Rasmussen PE, Yding Andersen C (December 2008). "True ovarian volume is underestimated by two-dimensional transvaginal ultrasound measurement". Fertil. Steril. 93 (3): 995–998. doi:10.1016/j.fertnstert.2008.10.055. PMID 19108822.
- ^ a b American Congress of Obstetricians and Gynecologists, "Five Things Physicians and Patients Should Question", Choosing Wisely: an initiative of the ABIM Foundation, American Congress of Obstetricians and Gynecologists, retrieved August 1, 2013, which cites
- U.S. Preventive Services Task Force (2004). "Screening for Ovarian Cancer: Recommendation Statement". The Annals of Family Medicine. 2 (3): 260–262. doi:10.1370/afm.200. PMC 1466669. PMID 15209204.
- Lin, Kenneth; Barton, Mary B. (April 2012), "Screening for Ovarian Cancer - Evidence Update for the U.S. Preventive Services Task Force Reaffirmation Recommendation Statement", AHRQ Publication No. 12-05165-EF-3, United States Preventive Services Task Force, archived from the original on 1 November 2014, retrieved 30 August 2013
- Partridge, E.; Greenlee, A. R.; Xu, R. T.; Kreimer, C.; Williams, J. L.; Riley, T. R.; Reding, B.; Church, C. C.; Kessel, J. L.; Johnson, C.; Hill, G. L.; Fouad, S.; Buys, L. R.; Isaacs, S. S.; Andriole, T.; Ogden, S.; Chia, D.; Ragard, L. R.; Prorok, P. C.; Gohagan, J. K.; Berg, C. D. (2009). "Results from four rounds of ovarian cancer screening in a randomized trial". Obstetrics and Gynecology. 113 (4): 775–782. doi:10.1097/AOG.0b013e31819cda77. PMC 2728067. PMID 19305319.
- American College of Obstetricians; Gynecologists Committee on Gynecologic Practice (2011). "Committee Opinion No. 477: The Role of the Obstetrician–Gynecologist in the Early Detection of Epithelial Ovarian Cancer". Obstetrics & Gynecology. 117 (3): 742–746. doi:10.1097/AOG.0b013e31821477db. PMID 21343791.
- ^ Seshadri, S.; El-Toukhy, T.; Douiri, A.; Jayaprakasan, K.; Khalaf, Y. (2014). "Diagnostic accuracy of saline infusion sonography in the evaluation of uterine cavity abnormalities prior to assisted reproductive techniques: a systematic review and meta-analyses". Human Reproduction Update. 21 (2): 262–274. doi:10.1093/humupd/dmu057. ISSN 1355-4786. PMID 25505226.








